Sourced from UHC broker email communication from 7/11/22:
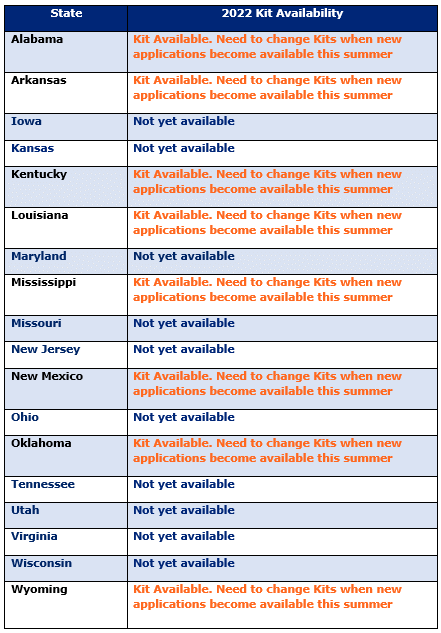
New Enrollment Kits and applications will be available and required soon for AARP® Medicare Supplement Insurance Plans, insured by UnitedHealthcare® Insurance Company (UHIC) and, where available, AARP® Medicare Supplement Insurance Plans, insured by UnitedHealthcare® Insurance Company of America (UHICA) in: Iowa, Kansas, New Mexico and Ohio.
The new applications will be required for plan effective dates of September 1, 2022, and later, and will be included in state-specific Enrollment Kits that will be available for the states noted above on August 26, 2022.
What to do Now
Existing Enrollment Kits can no longer be used after August 26, 2022, when the new Enrollment Kits and applications are available.
Please plan to download or order new Enrollment Kits on August 26, 2022. As of August 26, 2022, you need to use the new materials to ensure you have and are submitting the correct application.
What NOT to do Now
Do not order large amounts of Enrollment Kits now, as they will be outdated and the applications will not be the correct version as of August 26, 2022.
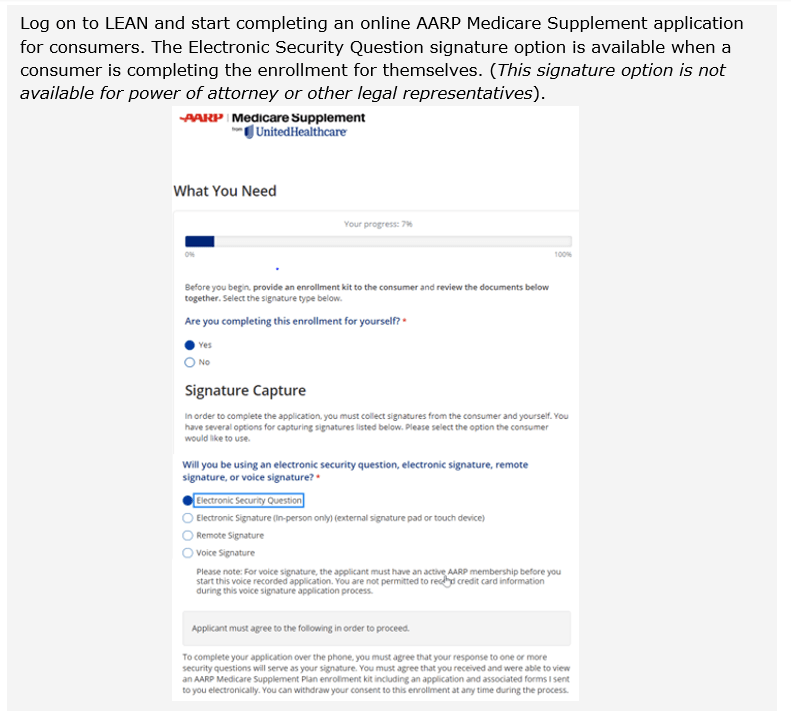
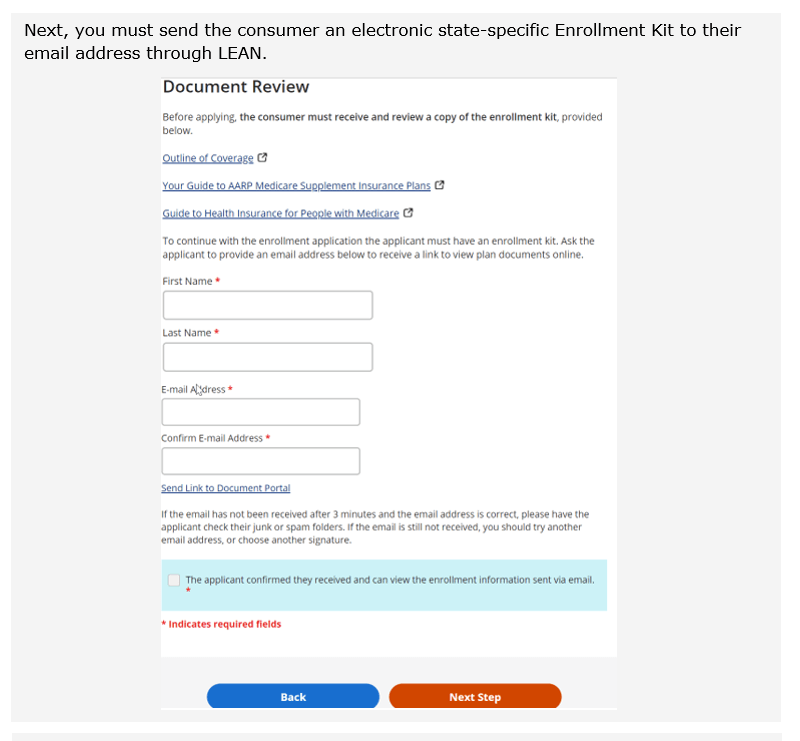
HELPFUL TIP! Use LEAN to submit applications and you’ll always have the correct applications!
If you have any questions, please reach out to your CSM rep.