Low Income Subsidy Plans Available to Help with Overall Health
WellCare communication from 3/15/21:
We wanted to remind you about the Low Income Subsidy (LIS) plans for beneficiaries with limited resources who DO qualify for the “Extra Help” subsidy, but DON’T qualify for a zero-dollar, dual special needs plan.
It’s important to remember that members receiving “Extra Help” (which helps with the Part D monthly premium, annual deductible, coinsurance and copayments) can choose any Centene plan with Part D, while the LIS plans work with the government’s Low Income Subsidy program. The low income programs help with prescription needs, so our LIS plans include other benefits to address our members’ overall health, like:
- Dental
- Hearing
- Vision
- Fitness
- And more
LIS Plans are available in the following Medicare markets:
Alabama, Arizona, Arkansas, California, Connecticut, Georgia, Illinois, Indiana, Kansas, Kentucky, Louisiana, Mississippi, Missouri, Nevada, New Jersey, New Mexico, New York, North Carolina, Ohio, Pennsylvania, South Carolina, Tennessee, and Texas.
If members are not already enrolled, they can apply for “Extra Help” in three ways:
- Online at www.socialsecurity.gov/extrahelp
- By calling Social Security at 1-800-772-1213 (TTY 1-800-325-0778) to apply over the phone or to request an application
- In person at their local Social Security office
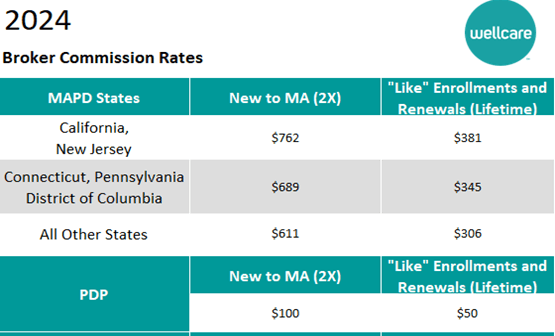
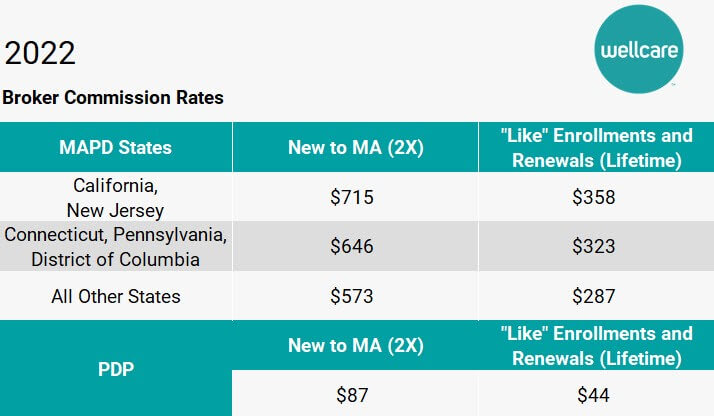
The LIS chart, available in Agent Connect and the Ascend portal, can help you understand the amount of “Extra Help” a beneficiary receives and help determine the right plan for them.
For more information, please see the 2021 Low Income Subsidy (LIS) Plans Product Video
If you have any questions on WellCare’s LIS plans contact your Cornerstone Senior Marketing representative.