Sourced from WellCare Broker Bulletin on 2.17.22:
We are getting close to the launch of the new Wellcare broker portal! As we wrap up the final stages of development, we would like to provide you with sneak peeks into what’s to come.
This Week’s Sneak Peek – Support Ticketing System
The ticketing system will offer several new enhancements that will provide you with better support from the Wellcare team.
As shown in the screenshot below, tickets will include the following:
- Inquiry Type and Subtype Categorization
- Detailed Description Related to the Inquiry
- Ticket Status
- Status Update Date
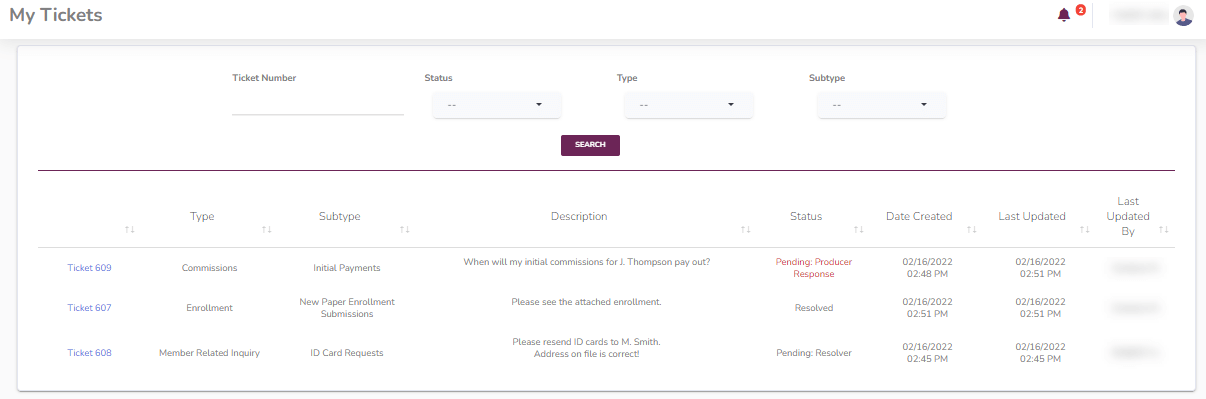
The search fields shown at the top make it easy to filter down to specific tickets based on Ticket Number, Status, and / or inquiry Type or Subtype.
Other features include email notifications to notify you when a ticket status has been updated, as well as a Pending Broker status to alert you the support team needs more information in order to resolve your escalation.
We encourage you to review the recently shared NEW Wellcare Broker Portal – Coming Soon! communication that provided additional information on key improvements and enhancements to support tickets, status and credential monitoring, commission statements, and dashboard reporting.
The new broker portal will be available soon! We appreciate your partnership and are excited to present you with a new tool that will aid in your success.
Remember, be on the lookout for more sneak peeks on the key features of our new broker portal!