WellCare 2022 Enrollment Tips & Reminders
Selecting the Correct Plan Year Application (2021 or 2022)
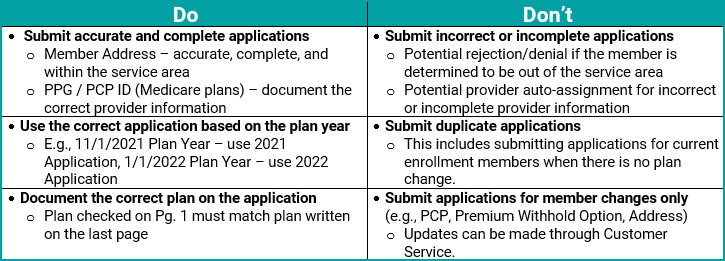
Plan year determines which application to use. Make sure to select the correct application based on the plan year of enrollment.
- 2021 Application – 11/1/2021 or 12/1/2021 effective date
- 2022 Application – 1/1/2022 – 12/1/2022 effective date
Note: Current members remaining in the same plan do not require a new application submission. Enrollment will continue into the new year.
Documenting the Correct Plan of Enrollment
- Select only one (1) plan on Pg. 1 of the application.
- The plan selected on Pg. 1 of the application MUST match the plan written on the last page.
If there is a conflict, the plan code/name documented on the last page of the application will take precedence.
Capturing Provider Information on Applications (Medicare Advantage plans)
Be sure to document accurate and complete Primary Care Provider information on applications to avoid auto-assignment of providers.
- PCP ID (WC) or NPI ID (CNC) must be on applications.
Note: If submission of IPA or PPG IDs is necessary for the enrollment, be sure to also submit the PCP/NPI ID and ensure they are valid providers for the plan.
Election Periods: Using AEP vs. SEP
For 2022 applications, you may notice that there is no longer a ‘check box’ to select AEP on the application. This is okay! As long as the Application Received Date is between 10/15/2021 – 12/7/2021 and the Requested Effective Date is 1/1/2022, the application will automatically process as the AEP option. If any SEP option is selected, the application process will use that SEP.
Additional Enrollment Reminders
Member Addresses – Accurate and Complete
Verify the members address and zip code to prevent enrollment rejections or denials if the member is determined to be out of the service area. Additional points to keep in mind regarding addresses:
- Street Name: Must be accurate, spelled correctly and in the right order
- Zip Code: Must be provided on all applications and accurate
- Rural Addresses: Must include the unit or space numbers
Member Changes Only – Provider, Premium Withhold Option, Address, etc.
- An application submission is not required for changes to a members address, provider or premium withhold option. Customer Service is available to assist with these type of changes.
Note: Pay special attention to the member’s provider and premium withhold option selected, and document accordingly.